Discharge follow-up. Referrals. Prior auths. Gap closure. Rely runs the calls and chart updates between every visit. AI for the routine work, our navigators for the exceptions, every step closed in your EHR.



















Up to 90% of ED patients leave without structured follow-up. More than half of specialist referrals never stay in network. The fastest-growing job description in your system is "navigator" and you still can't fill the seats. Software alone hasn't moved the numbers.
Pure software hits a ceiling on exceptions. Pure outsourcing scales headcount and stops there. Rely runs all three layers, so every exception our team resolves becomes the next automation, and your nurses never get the queue back.
Voice and text agents handle outreach, intake, scheduling, and follow-up, 24/7. They read and write in your EHR, follow your clinical protocols, and escalate to a human the moment a case stops being routine.
When the AI hits an exception, a Rely navigator picks it up with full context, in the same conversation. The patient stays in our system. Your nurses don't see the queue.
of incoming calls fully resolved by AI, no callback. Large California county hospital, 120-day review.
Every exception our navigators close becomes a labeled training example. Patterns turn into workflows. Workflows turn into new agents. The system gets cheaper the longer it runs.
Every program ships with the agents, navigators, dashboards, and integrations to go live in weeks. Pick one. Add the rest as you scale.
Reminders, prescription verification, follow-up booking, and a navigator on standby for the cases that need a person. Runs alongside your existing care team, inside your EHR, with results visible from week one.

When the AI hits a wall, the call doesn't drop into your nurse's in-basket. A Rely navigator picks it up, with full context, in the same conversation.
Every program is staffed by clinically-trained navigators working alongside the AI. They handle exceptions, retrain the agents, and stay with patients through the hard cases that software alone can't close.
Numbers from live programs. Every metric is auditable in our customers' systems. Named clinical references on request.
No 18-month Epic project. No army of consultants. We bring the agents, the navigators, and the integrations. Your team approves the scope and the scripts.
We meet your team. One Markdown file defines program scope, payer rules, EHR access, escalation paths. No HL7. No IT ticket.
We build the voice agents to your protocols and connect to your EHR with role-based credentials. Your team reviews every script before go-live.
Agents run on real cohorts in supervised mode. Our navigators handle every exception. Your team sees every call, every write-back, every handoff.
Production. AI handles routine work 24/7. Our navigators work the exceptions. Weekly dashboard, monthly review with your team.
Most AI vendors finish the call and hand the queue back to your nurses. Most BPOs scale headcount and call it a day. We own the work end to end. Agent. Navigator. EHR write-back. Escalation. Until it's closed and charted.
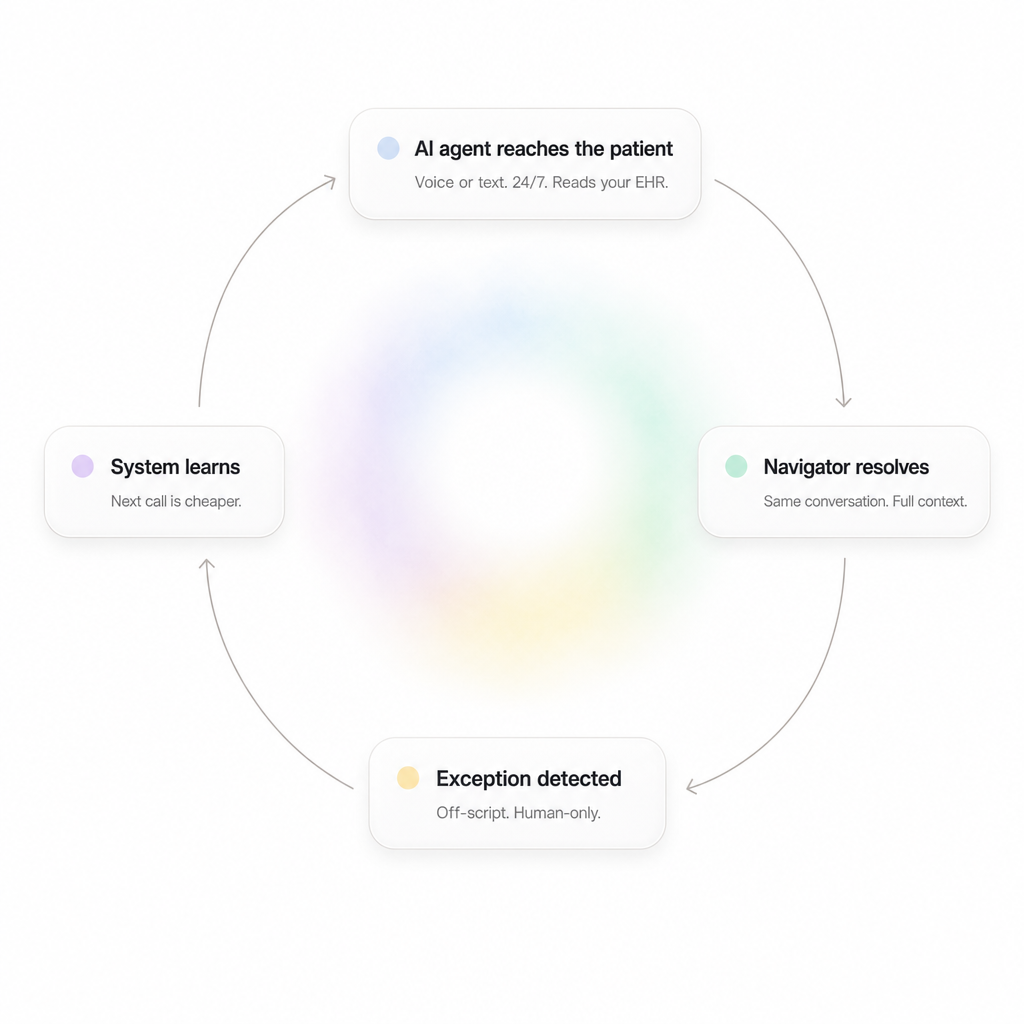
When something falls outside the script, our navigator picks it up. Not someone on your floor. The patient stays inside our system, the work stays with our team.
Every exception our navigators resolve becomes the next automation. Same contract, fewer minutes of human time every quarter. The economics improve while you sleep.
A weekly dashboard for ops. A monthly review with your team. Capture rate, outcomes, dollars. Every call written back to your EHR.
HIPAA-grade infrastructure with full BAA coverage. SOC 2 compliant, monitored continuously by Vanta. PHI minimization, audit trails, and access controls across every agent run.
Read and write directly into any modern EHR. Epic, Cerner, athena, eClinicalWorks, Meditech, NextGen and others. No HL7 build, no IT ticket.
Every clinical exception routes to a trained Rely navigator. AI only handles what AI can finish. Patients always reach a person when it counts.
30 minutes with our team. We'll show you a real program running today: real calls, real EHR write-backs, real exception handoffs. No mocked data.